Fungal acne looks a lot like hormonal acne or bacterial acne, but the culprit isn’t the same as other types of acne. Instead, it is an overgrowth of yeast that hangs around in the hair follicles. The technical term: pityrosporum folliculitis or malassezia folliculitis.
Malassezia actually lives on everyone’s skin, Joshua Zeichner, the director of cosmetic and clinical research in dermatology at Mount Sinai Hospital in New York City, adds. However, yeast levels tend to increase during hot, humid weather or when you’re sweaty. “High yeast levels promote inflammation, which, in turn, manifest on the skin as pus bumps,” Zeichner explains.
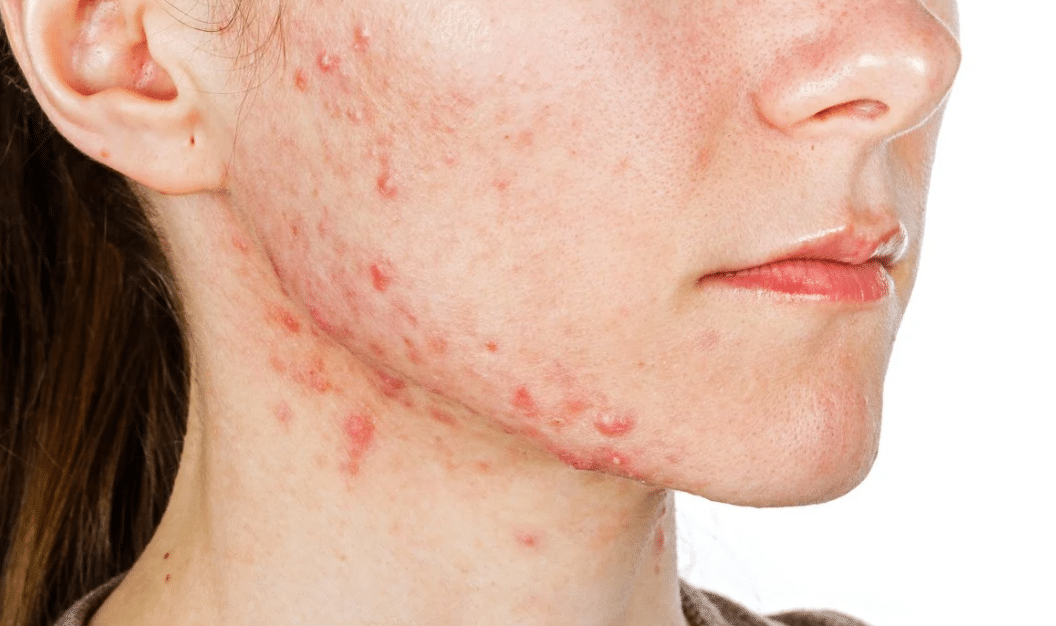
Fungal acne appears as inflamed, itchy, acne-like eruptions that are really pus-filled bumps. It shows up as breakouts in areas where you typically have a lot of oil — in your T-zone (forehead, nose, chin), chest and back. The telltale difference is that fungal acne can be itchy, and regular acne is not. Other clues: fungal acne is generally uniform in size and shape, and appears in clusters of small whiteheads.
How Is It Different From Other Forms Of Acne
Well, fungal acne is not acne at all. Zeichner says it’s truly an infection of the hair follicle. Some other differences include intense itching and placement. “Inflammatory acne tends to affect the face and is usually either due to increased oil production, follicular plugging, excess bacterial growth of propionibacterium acnes, or hormonal changes,” Idriss says. “Fungal acne, on the other hand, frequently appears as uniform papules and pustules on the chest and back or in areas of occlusive clothing.”
What Does Fungal Acne Look Like
Despite its resemblance to bacterial acne, fungal acne is actually caused by yeast (yes, a fungus) that inflames the hair follicles on your skin and causes pimplelike bumps. The condition is technically referred to as pityrosporum folliculitis or malassezia folliculitis, for the specific type of fungus (malassezia is the more updated term, but your dermatologist may still call it pityrosporum).
Read Also: Closed Comedones Extraction
Antibiotics aren’t the only factor in developing fungal acne—sometimes our own habits are the culprits. For instance, wearing tight, nonbreathable clothes often contributes to breakouts, Dr. Chung says. More specifically, wearing sweaty workout clothes for too long or wearing fitness gear without washing it can create a very hospitable (read: moist) environment for fungi to grow, Emily C. McKenzie, MD, clinical instructor in the department of dermatology at the University of Utah, tells SELF.
Fungal Acne Treatment
An antifungal is needed to treat pityrosporum folliculitis. An oral antifungal, such as itraconazole or fluconazole is used. These antifungals are off-label treatments trusted Source because they’re not FDA-approved for this specific condition. Topical treatment with an antifungal shampoo can also be used in those who don’t want or cannot tolerate oral antifungal treatment. If you’d like to treat pityosporum folliculitis at home, there are several products and home remedies you can try.
- Bioderma Sebium H2O Micellar Water, $15: This micellar water contains anti-fungal powerhouse, sulfur, making it the perfect first step of your nighttime routine. Not only will it help the infection, but it’ll also help balance oil production while removing your makeup.
- Neutrogena Body Clear Body Wash, $8: If you’re prone to fungal acne on your chest or back, this product should be at the top your list. The formula contains 2% salicylic acid; a potent BHA that’ll exfoliate the skin and dissolve the glue that binds dead skin cells, which block your pores. It’ll also help lower oil production, and as it has anti-inflammatory properties it’ll soothe existing spots. Once you’ve massaged it onto damp skin, massage it in for one minute.
- Nizoral A-D Anti-Dandruff Shampoo, $14: This anti-fungal shampoo is often prescribed to treat bad cases of dandruff and seborrheic dermatitis as it kills the fungal growth. Apply a dime-sized amount to the area and let it sit for two minutes before rinsing. You can also use other anti-dandruff shampoos like Selsun Blue or those that contain ketoconazole.
Fungal Acne Vs Bacterial Acne
When bacterial begins to grow in clogged follicles, it creates blackheads or whiteheads on the surface of the skin. Hormones, oral contraceptives, diet, environment, and a range of other situations can lead to the development of bacterial acne. Luckily, it’s treatable! Washing your face with over-the-counter acne treatments, ensuring you eat a healthy diet, and washing off makeup at the end of the day all help to treat acne. A dermatologist can also help if necessary.
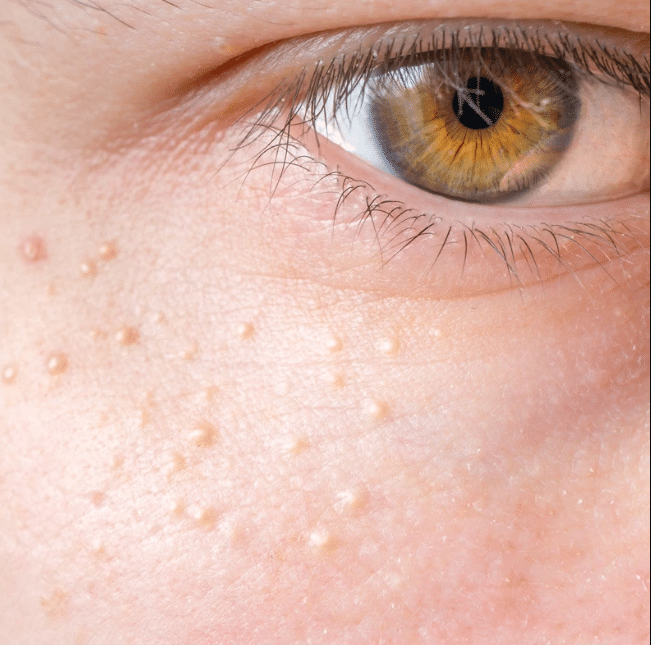
Although fungal acne has been deemed so, it only gets its name because it so closely resembles a traditional acne breakout. In reality, fungal acne isn’t an acne breakout at all! It’s caused by yeast in your skin that becomes trapped in your skin’s hair follicles and causes small, pimple-like bumps. The technical name for this medical condition is malassezia folliculitis or pityrosporum folliculitis, depending on the specific type of yeast fungus.
Is Salicylic Acid Good For Fungal Acne?
Salicylic acid is anti-inflammatory, keratolytic (helps exfoliate dead skin cells), anti-fungal and anti-bacterial. It penetrates pores to loosen clogged follicles by breaking apart dead skin cells, softening them, and helping them slough off the skin.
Is Honey Good For Fungal Acne?
You can use honey as a cleanser to help prevent breakouts because of its antibacterial and anti-fungal properties. For a more potent effect, honey can be left on breakouts to help them heal faster.
Read Also: How Long Does Ruptured Ovarian Cyst Pain Last
How Is Malassezia Treated?
In general, malassezia infections are treated with topical or oral antifungal agents, such as ketoconazole shampoo and oral fluconazole. Seborrhoeic dermatitis may also treated with topical steroids.
What Triggers Fungal Acne?
What causes fungal acne? Despite its resemblance to bacterial acne, fungal acne is actually caused by yeast (yes, a fungus) that inflames the hair follicles on your skin and causes pimplelike bumps




